Friday Author: Seth Kaplan
The headline for this article in the 2/16/16 Wall Street Journal reads, “Hospitals Unite to Defeat a Common Foe: C Difficile.” The subhead continues, “When it comes to safety, health-care providers are finding collaboration must replace competition.”
 Each time a story like this one appears, my frustration level goes up. Why? Because solutions to the problem of hospital-based infections have been used for at least 75 years here in the United States,
Each time a story like this one appears, my frustration level goes up. Why? Because solutions to the problem of hospital-based infections have been used for at least 75 years here in the United States,
Abroad, many people are trained in these techniques, yet health-care professionals often are unaware that these solutions exist.
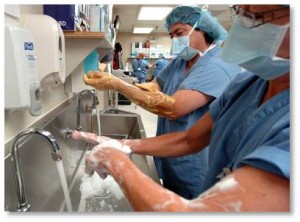
Hospital-Based Infections
The article’s subhead expresses a correct thought, which would be even more complete with the addition of the word “communications.” Siloing knowledge almost never leads to creative, workable solutions, especially in the field of hospital-based health care. But reinventing the wheel to knock out the same infection each time it spreads throughout a hospital wastes time, money, and human resources.
That doesn’t’ take into account the wellness of patients and health-care workers who sicken and sometimes die as a result of contracting hospital-based infections such as C. Difficile, MRSA (Methicillin-resistant Staphylococcus aureus), Legionnaire’s Disease, and any of the other infections that periodically plague (pun intended) hospitals and other health-care settings.
The Answer? SQA—Statistical Process Control
First, a little history. After World War II, the United States, in addition to organizing the Berlin Airlift, sent many professionals to Japan to reconstruct their heavy and light industries, which had been destroyed during the war. Two of the men assigned to this task, W. Edwards Deming and Joseph Juran, taught the Japanese manufacturing executives SPC, or statistical process control (also called SQC, statistical quality control).
The definition of quality is no different today than it was then: Conformance to specifications. When you think about it, quality is free! If the process conforms to all specifications without exception or error, then there are no rejects.
How Does This Approach Work In Practice?
 I learned this approach many years ago, when I worked at Texas Instruments (TI) in Attleboro, MA. All exempt employees were trained by top management in these principles and how to use them.
I learned this approach many years ago, when I worked at Texas Instruments (TI) in Attleboro, MA. All exempt employees were trained by top management in these principles and how to use them.
At the end of the classroom training, management established multidisciplinary teams and assigned each one a real problem to solve.
My team consisted of me (marketing communications) and people representing finance, engineering, manufacturing, etc.; about eight in all. Our problem: The epoxy on the automotive chokes sold to GM, Ford, and other companies was failing a percentage of the time, causing customers to reject shipments based on random sampling.
The tools we used fell into one of four areas of Root Cause Corrective Action, also known as Cause and Effect Analysis:
- Identify the problem
- Diagnose the cause
- Remedy the cause
- Hold the gains
To cut to the chase, our team interviewed people at every stage of the sourcing and manufacturing process. Knowing that TI made these chokes at other plants in other countries, we talked to the production people at these locations; i.e., we communicated with them.
Lo and behold! Their epoxy came from a different supplier, one that had overcome the adhesion problem. Once another source provided epoxy to the Attleboro operation, the problem was solved.
Now You Can See . . .
. . . how hospitals can use this approach to identify the sources of infections (it often turns out to be something simple, like washing hands more often. Imagine, health-care professionals NOT washing hands between patients and procedures), understand the chain of events and contacts that leads to the spread of the infections, rework their processes and train all staff to follow the new protocols, measure the results, and, most importantly, maintain the gains over time.
 I wrote to Atul Gawande, the surgeon and brilliant writer for The New Yorker magazine, about this body of knowledge just before his book, The Checklist Manifesto, came out a few years ago. He and I have, as Facebook might put it, common acquaintances, so I thought he might write back. No such luck.
I wrote to Atul Gawande, the surgeon and brilliant writer for The New Yorker magazine, about this body of knowledge just before his book, The Checklist Manifesto, came out a few years ago. He and I have, as Facebook might put it, common acquaintances, so I thought he might write back. No such luck.
His basic premise is that the use of checklists can help eliminate mistakes and increase productivity and safety in many different work environments. As well-thought out and common sense as his thesis is, if he had known about and included the information I describe here, his recommendation would have been more comprehensive and effective.
Communications and Collaboration
In my opinion, one-step-forward-and-two-steps-back is not an effective way to create and maintain safe environments in hospitals, nursing homes, and other health-care locations. Communication and collaboration are the keys to effecting permanent, measurable, repeatable change.
